
Though the average person knows little about histamine besides the commonly prescribed “antihistamine” for seasonal allergies, they can cause many serious issues in those with a compromised body. Because of the damage done through untreated, Chronic Lyme Disease, my body has become overrun with this important, yet very annoying compound that my cells are constantly releasing. Despite what the results of any allergy blood test may or may not show, those with overactive histamine tend to react to practically anything from taste, touch, and even smell. However, most doctors do not seem to take the statement “I’m allergic to everything” very well, and most people are left to deal with the debilitating symptoms alone.
Note: simply click on highlighted words for more info
What is Histamine?
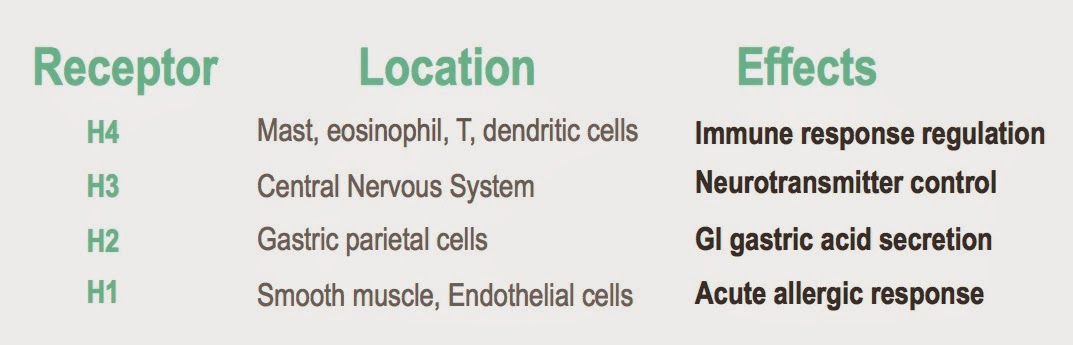
H2
H3
H4

DAO
Treatment

Ephesians 2:10 “ For we are God’s masterpiece. He has created us anew in Christ Jesus, so we can do the good things he planned for us long ago”

Let me just say, THANK YOU (and WOW!) I’m going to have to study back through this (!) but you’ve brought me to a m-u-c-h deeper 🙂 understanding of my autoimmune condition, and I am so grateful to you! Keep fighting the good fight, Gabriella! 🙂
An incredible investigation Gabrielle!
I would add cultivated ghee to my diet but I have read that is fermented … Do you think it could give me problems with histamine? Thanks!
Hello, I’m interested in your Dr.’s protocol for different Chinese herb combinations in pill form. herbal tea, specific bath salt remedies, and morning/night cream supplements. The FAHF-2 (Food Allergy Herbal Formals)
Would you be willing to share the specifics and who your Dr is, to see if she might be in my area.
Thank you!
Hi Tamara,
Please send me an email ([email protected]), and I can refer you to some links, as well as the names of the doctor!
I would also be interested in the links for the Chinese herbal formulas and list of practitioners. Great article on histamine which I suffer from. My 25 yr. old daughter found out in Dec. she has advanced LD and I have been suspicious she could also have the histamine issue. Thanks, Denise
I did an elimination diet, and realized histamine is a HUGE issue. Health has been going down hill the last five years. Tested positive for Lyme bands. IYO, would you push more focus on histamine or Lyme? Thanks for your time!! 😉
For me, the histamine issue is a result from Lyme…However, simply addressing the Lyme did not get rid of the histamine problem, since there was a bunch of healing to do regardless of if the Lyme was under control or not. It really seems like it is different for everyone, and sadly (as always) takes a bit of experimentation.
Thanks for all the info! I’m on a strict AIP lifestyle and a low histamine diet. I too rotate my food intake to avoid food reactions. It’s tough! I try to read something new about my diseases/disorders each day to constantly grow in knowledge so I can take better care of myself and my family. I found you today!
Wow! This was soooo good! Thank you so much! I had a somewhat understanding, but this really helped me get a fuller picture! I am in reaction mode and can’t get out 🙁 I am so grateful to know that God knows my deepest needs and this comes as no surprise to Him. I am resting in His grace and praying for wisdom and clarity (and pollen season to end quickly 🙂 Our bodies are amazing and resilient and can be healed naturally if we know what they need! The not knowing is the hardest part 🙂
Hi just wondering if you get a histamine detox or a ramping up of your symptoms when you start taking Quercetin as there so much histamine in the body to be released?
Hi Kaylia,
I have not personally experienced this…
Very interesting. Who is the author of this particular information?
The authors are cited through the various linked words or phrases throughout the article.
Thank you SO MUCH for distilling this. And I mean that. I waded through a large, detailed paper describing histamine receptors and cites and cells and all that. So much that I can’t remember the important stuff. But this is great. Definitely pinned for reference.
Through much trial and error, I’ve found that histamine is the key to my chronic eczema. And now that I have a handle on mine, I’m hoping to be able to help my daughter more, as well.
Thank you for this article and everyone’s comments along the way. I have a long history of complementary health interest and use some 38 years; added to a nursing background and a love of how the body works … over the past 13 years I have seen leaky gut and eczema symptoms disappear by giving the body more of what it needed and less of the other stuff. I have also recently added in a practice of ‘ The Healing codes ‘ from a book by Dr Alex Lloyd where the body can be refired to do its work … believing this could help to add to the other good work … involves Body Soul and Spirit
Great article …I too suffer from these symtoms..I have mast cell activation syndrome…..are there any h3 supplements out there ?
Thanks
Lisa
Thank you so much for your post. I got an Aeromonas infection in February that knocked me off my feet for 4 weeks, I have never been so sick in my life. 6 weeks after that I developed severe pressure in my head and constant sinus swelling that no-one can explain. I am always flushing and reacting to everything. My arthritis has kicked up and I now have huge amounts of inflammation. I just seem to react to everything, I can no longer eat avocado’s or other high histamine foods since catching the Aeromonas. I have been convinced I have a histamine problem but no-one really understands how that could be. I am so sick and tired of constant pressure in my head, facial flushing, and swelling in my sinuses, sometimes I find it hard to breathe or swallow. My GP is coming around to the idea that it could be a histamine reaction but doesn’t know why. I am sure it was the Aeromonas. Sorry for the ramble, it’s just your article was the first time I saw Histamine and Aeromonas linked in an article. Wishing you all the best.
I have what I believe to be late Lyme disease, possibly brought on by one or more drugs I was given during surgery last year. I’d like to know if the B. Burdgorferi bacteria are stimulated or activated by histamine. If so, it could explain why my symptoms arise every morning soon after I wake up.
If anyone has any information on this, or can point me to a study, I would appreciate it.
Fabulous article! Now my main question: What are the best testing factors for MCAD and are they reliable?
I too have chronic Lyme and just recently began having instant/severe anaphylatic reactions to basic foods I never had a problem with before. I have started taking measures as quickly as possible to “remedy” this situation as I do not want to let it get out of control as so many other things have in the last few years. So far, I am taking bee pollen, raw honey, and nettle leaves to attempt to control the histamine reactions (I’ve definitely noticed a difference but I have also been extra cautious with what I am eating).
My insurance doesn’t cover a lot of practices and the practices versed in MCAD in my area do not accept my insurance, hence I am trying to find the best way of testing?
So what kinda herbs was in these pills you speak of is what I wanna know!!! Lol
Hello, My daughter has Lyme and histamine issues for about 15 years – After seeing many doctors and having surgery, we only discovered that the real problem was Lyme about two years ago. Nothing has slowed down her histamines. Was your immunologist’s tea able to help you control your histamines? Are there DAO and HMT supplements that can help with the overactive Lyme-related histamines issues?
Thank you for this information. This article has been so helpful.I would really appreciate knowing what herbal treatments you have been doing also.
Thank you
Thank you so much for this excellent article! With the cognitive issues from CLD and histamine issues, it’s so wonderful to have your simplification of this complex issue.
I have recently put all the puzzle pieces together to realize that I have histamine issues (likely linked to antibiotics used as well as genetic predisposition) and have spiraling allergic responses, eg vertigo from congestion build up that I don’t notice until it’s too late that happens with almost any exposure to pollen, convulsions/tremors with consciousness that can last for hours after use of prescription drugs such as tramadol or pain killers (note: one short online search shows that opioid analgesics are histamine releasing, yet doctors just look at me blank- faced when I tell them the reactions I’ve had), and similar convulsions but for shorter time of under an hour after exposure to histamine inducing events including being pricked on forearms by weeds, chemical smells in dentist office and eating and smelling chile. I already have been on a somewhat limited diet for years, e.g dairy and gluten free, no refined sugar and low sugar, etc. along with other measures such as supplements, acupuncture, naturopath etc. yet my symptoms continue to worsen. I briefly considered implementing a low histamine diet, but when I saw foods on the no list such as avocados, I thought, ” When does this end? Eating a restricted diet is helpful, but at what point will the bubble be too small to live in?” With a stroke of grace in my continual digging and reading, I found a website by a homeopath named Joette Calabrese (you can search by her name) who seemed to have a similar path. I am just beginning to learn, but practical homeopathy is what is turning this around for me. I have had several successes just by studying her free online blogs and podcasts. She has even published the homeopathic remedy protocol for Lyme disease. It is worth learning about because it has and will continue to change my life into one that I’m able to live more fully.
Additionally, Thank you for this article! Very helpful.
Has the Chinese medicine tea and FAHF-2 helped you??
I was introduced to the concept of Histamine Intolerance in an Face Book Atrial Fibrillation Support group. Histamine intolerance was mentioned as a catalyst for heart beat Irregularities. I was eating a lot of the foods that are on the histamine avoid list daily like strawberries, spinach, tomatoes, avocados, walnuts, sunflower seeds, dried fruit, aged cheese and wine to name a few. Since I have been on the elimination diet I have only had afib when I tried to introduce sunflower seed and dried fruit back into my diet. I was surprised that heartbeat irregularities was not included in the symptom list in this article. I have seen it listed in other articles and I am happy that the elimination diet works for me.